𝐔𝐓𝐄𝐑𝐈𝐍𝐄 𝐅𝐈𝐁𝐑𝐎𝐈𝐃𝐒:
Uterine fibroids, or leiomyomas, are the most common benign tumors of the uterus, originating from the smooth muscle layer (myometrium) and connective tissue of the uterus. They affect many women during their reproductive years and vary greatly in size, location, number, and symptoms. Here’s a detailed breakdown:
Pathophysiology and Development of Uterine Fibroids:
Fibroids develop when a single smooth muscle cell in the uterus multiplies rapidly, forming a mass. The exact cause is unknown, but fibroids are hormone-dependent, particularly influenced by estrogen and progesterone. These hormones stimulate the growth of fibroids, making them larger during pregnancy and often shrink after menopause when hormone levels drop.
Fibroids can also be influenced by genetic changes, with mutations in specific genes contributing to abnormal cell growth. Additionally, certain growth factors (like insulin-like growth factors) and extracellular matrix components (collagen, fibronectin) play a role in their growth and structural integrity.
Types of Uterine Fibroids:
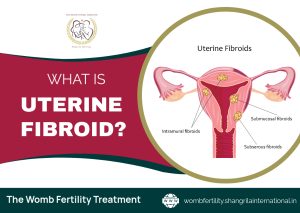
Fibroids are categorized based on their location within or around the uterus:
1. Intramural Fibroids:
o Develop within the muscular wall of the uterus.
o Most common type of fibroid.
o Can grow large and distort the shape of the uterus.
o Often associated with heavy menstrual bleeding and pelvic pain.
2. Subserosal Fibroids:
o Grow on the outer surface of the uterus.
o These can develop a stalk (pedunculated fibroid) and may extend into the abdomen.
o Less likely to affect menstruation but can cause pressure on nearby organs, such as the bladder or intestines, leading to urinary or bowel issues.
3. Submucosal Fibroids:
o Develop just beneath the uterine lining (endometrium).
o The least common type but often cause significant bleeding and fertility problems.
o Even small submucosal fibroids can cause disproportionately severe symptoms.
4. Pedunculated Fibroids:
o These fibroids are attached to the uterus by a stalk-like structure (either subserosal or submucosal).
o They can twist (torsion), causing sharp pain, requiring emergency treatment.
5. Cervical Fibroids:
o Rare fibroids located in the cervix (the lower part of the uterus).
o Can block the cervical canal and impact menstrual flow and intercourse.
Size and Growth:
• Fibroids can range from microscopic sizes to as large as grapefruits or even larger.
• Some grow slowly, while others can increase in size rapidly.
• Their growth can be influenced by hormonal levels (e.g., pregnancy causes them to grow, while menopause often shrinks them).
Symptoms of Uterine Fibroids:
The symptoms of fibroids depend largely on their size, number, and location. Many women with fibroids experience no symptoms, while others may face the following issues:
1. Menstrual Changes:
o Heavy, prolonged menstrual bleeding (menorrhagia).
o Passage of blood clots during menstruation.
o Irregular periods or spotting between periods.
o Anemia due to excessive blood loss, leading to fatigue and weakness.
2. Pelvic Pain and Pressure:
o Constant pelvic pain or a feeling of pressure.
o Lower back pain, often radiating down the legs.
o Pain during intercourse (dyspareunia), especially with deep penetration.
o Acute pain if a fibroid outgrows its blood supply, leading to degeneration.
3. Bladder and Bowel Symptoms:
o Frequent urination or difficulty emptying the bladder completely (due to pressure on the bladder).
o Constipation or bloating due to pressure on the rectum.
o Difficulty with bowel movements.
4. Reproductive Complications:
o Infertility: Submucosal fibroids can interfere with embryo implantation.
o Pregnancy complications: Miscarriage, premature labor, or the need for a cesarean section.
o Pain during pregnancy: Fibroids often grow in response to increased hormone levels.
o Postpartum hemorrhage due to poor uterine contractions.
5. Abdominal Enlargement:
o As fibroids grow, they can cause noticeable abdominal swelling, mimicking pregnancy.
Causes and Risk Factors:
While the exact cause of fibroid development remains unclear, the following factors have been linked to their growth:
1. Hormonal Factors:
o Estrogen and progesterone stimulate fibroid growth. This explains why they are common during the reproductive years and often shrink after menopause.
2. Genetic Predisposition:
o A family history of fibroids increases the risk.
o Certain gene mutations have been identified in fibroids.
3. Other Risk Factors:
o Race: African-American women are at a higher risk, tend to develop fibroids at a younger age, and often experience more severe symptoms.
o Early menarche (first menstrual period before age 10).
o Obesity: Higher body weight is associated with increased estrogen levels, promoting fibroid growth.
o Diet: High consumption of red meat and low intake of green vegetables, fruit, and dairy have been linked to a higher risk.
o Vitamin D deficiency.
Diagnosis:
• Pelvic Examination: Large fibroids can often be detected during a routine pelvic exam due to an enlarged or irregularly shaped uterus.
• Ultrasound: The most common diagnostic tool, particularly transvaginal ultrasound, which allows detailed imaging of fibroids.
• MRI: Useful for determining the size and location of fibroids and distinguishing them from other uterine masses, such as adenomyosis or cancer.
• Hysteroscopy: A procedure where a thin, lighted scope is inserted into the uterus to view the inner surface, especially useful for diagnosing submucosal fibroids.
• Sono hysterography: A specialized ultrasound where saline is injected into the uterus to better visualize the fibroids.
Complications of Uterine Fibroids:
• Anemia: Due to chronic heavy menstrual bleeding.
• Pregnancy Complications: Higher risk of miscarriage, preterm labor, placental abruption, and cesarean section.
• Infertility: Especially in cases of submucosal fibroids.
• Bladder or kidney damage: Large fibroids can compress the urinary system, leading to kidney damage over time.
Understanding fibroid and getting the appropriate diagnosis is crucial for managing symptoms and improving quality of life. If you’re experiencing symptoms or considering treatment, consulting with a healthcare provider who can tailor the management plan to your specific condition is essential.

